NIPT test (Non-Invasive Prenatal Test)
Shortly after 2000, the HUman GEnome project (HUGO) succeeded in semi-automatically analyzing sections of the human genetic material DNA using what is known as massive parallel sequencing and thus decoding the human genome.
Since DNA of the unborn child (so-called cell-free DNA) also circulates in the blood of a pregnant woman, it has been possible since 2012 to deduce the genetic characteristics of the child from a simple blood sample from the 10th week of pregnancy. The effort required for this so-called sequencing is enormous, both in the laboratory and in the computer-assisted evaluation, which is why only specialized laboratories can make the corresponding investments. The procedure is also known as NIPT (non-invasive prenatal testing).
If, after counting millions of fragments, chromosome 21 is overrepresented, this allows the conclusion with a high degree of certainty that the unborn child has three instead of two copies and thus has trisomy 21 (Down syndrome, formerly called mongolism).
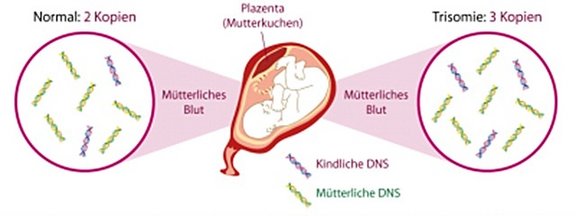
Left: maternal blood with chromosomes of the mother (green-yellow) and normal proportion of fetal chromosomes 21 (red-blue). Right: In an unborn child with trisomy 21, an excess of fetal (red-blue) chromosomes No. 21 is found in the mother's blood.
TESTS OFFERED BY OUR PRACTICE GROUP
NIPT from the University of Zurich:
Is based on Illumina® high-throughput sequencing technology:
- Basic Trisomy NIPT (Illumina-VeriSeq® NIPT-Solution): covered by basic insurance under certain conditions for trisomies 13, 18, and 21. This NIPT detects with high probability the most common fetal trisomies 13, 18, and 21, as well as, if desired, variations in the number of sex chromosomes X and Y (e.g., Turner or Klinefelter syndrome), and determination of the child's sex. Cost: 510 CHF.
- Extended NIPT for all visible chromosomal defects (combined Illumina VeriSeq® and internal IMG NIPT): in this combined extension NIPT, all chromosomes (1-22, XY) are examined for trisomies and monosomies as well as for major deletions and duplications. Cost: Additional charge of CHF 350 (not covered by basic insurance).
- In the case of twin pregnancies and egg donation, both tests are also informative.
Panorama test (Genetica laboratory, Zurich / Natera, California)
examines only particularly significant portions of the chromosomes (SNPs, single nucleotide polymorphisms) and compares them with those of the mother.
- Basic examination: trisomies 21, 18 and 13, triploidy, Turner syndrome. Cost 660.-- Fr. NEW since July 2015: The basic examination is covered by health insurance if the first trimester blood test showed a trisomy risk higher than 1:1000. Otherwise, the supplementary insurance may make a voluntary contribution.
- Additional testing since July 2014: Test for so-called microdeletion syndromes (DiGeorge, Prader-Willi, Angelman, Cri-du-chat, 1p36). Cost additional 250.-- Fr. The five microdeletion syndromes tested are severe and affect a total of one in a thousand newborns. Those who decide to have a new blood test will in the majority of cases also want this additional examination, unless they only want to exclude trisomy 21.
- Also possible in twin pregnancies and pregnancies with donor egg.
NIPTEST - FACTS - AND OPEN QUESTIONS
In principle, the tests represent considerable progress and expand the so-called non-invasive (without puncture needle and thus without residual risk of miscarriage) detection options of hereditary disorders. Experts now agree that all pregnant women need to be educated about the availability of NIPT.
- Testing can be ordered from 9 to 12 full weeks of pregnancy and takes about two weeks. For the time being, the costs (see above) are not covered by health insurance (please check if your supplementary insurance voluntarily covers part of the costs). It detects 98-99% of cases of trisomy 21, but not all; in particular, so-called mosaic trisomies are not detected. The method also cannot currently be used for twins. In any case, an abnormal test result should be verified by amniocentesis (next chapter).
- A NIPT test does not replace detailed ultrasound at 11-14 weeks. In particular, measurement of nuchal translucency (NT, previous chapter) is still useful because this warning sign may indicate problems other than trisomy 21. We usually recommend that the ultrasound with NT measurement be performed first, just to determine if the pregnancy is still okay. Only then we will decide together with the pregnant woman how to proceed (conventional first trimester blood test, new blood test with costs, directly amniocentesis or no further examinations).
- The new blood tests were developed and reviewed for high-risk pregnant women. Young pregnant women with normal nuchal translucency are at such low risk that the new blood test may give almost as many false positives as it detects actual problems. Young pregnant women with normal nuchal translucency are therefore more likely to be recommended the conventional first trimester blood test in the first instance - not only because of the cost savings; however, we will always grant the informed request for direct NIPT.
- In the medium term, it will be possible to detect more and more hereditary disorders using the same technique. As the availability of the test increases and costs decrease, the test is likely to be covered by health insurance (resulting in a net cost saving for health insurers because fewer amniocenteses and chorionic biopsies are expected). Medical consultation at the beginning of pregnancy has undoubtedly become even more complex and time-consuming.
- Our community of practice has been offering the new blood tests in collaboration with our partner laboratories since 2012.
NIPT TEST - ETHICAL CONSIDERATIONS
Our society says a broadly supported yes to prenatal testing (and thus, in the final analysis, to abortion in the case of a sick child). Distribution disorders of the genetic material such as trisomy 21 depend massively on the age of the mother, which is why many older mothers are in great concern whether their unborn child is healthy. However, all examinations (ultrasound, blood test, amniocentesis) are completely voluntary, and a minority would forego them and accept a handicapped child (which we respect, of course). It is the old contrast between "being in good hope" and "expecting a (healthy) child".
The blood test does not bring anything fundamentally new in this respect, except that the examination for trisomy 21 becomes even easier. Ethicists therefore fear that - if fewer and fewer children are born with trisomy 21 - these people will be pushed even further to the margins of society. In our opinion, the informed pregnant woman should be free to decide which examinations to take, and respect for disabled people should not depend on their number.
Contact
GYNÉ LANG
Kohlrainstrasse 10
8700 Küsnacht (Zurich)
Phone +41 44 912 25 25
praxis@gynelang.ch
Opening hours
| Monday | 08.00 - 12.00 | 13.30 - 16.30 |
| Tuesday | 08.00 - 12.00 | 13.30 - 16.30 |
| Wednesday | 08.00 - 15.00 |
| Thursday | 08.00 - 12.00 | 13.30 - 16.30 |
| Friday | 08.00 - 15.00 |
![[Translate to English:] Frauenarzt Zürich [Translate to English:] Frauenarzt Zürich](/fileadmin/sites/gynelang/media/gynelang_logo.png)